Financial stress is a barrier to care, and it’s quickly getting worse.
Common mental health issues like depression and anxiety have risen around 10% since 2025.
While 60% of U.S. adults report that mental health has become more important to them, access to mental health services has declined, with 52.6% never trying services like talk therapy or psychiatry.
“You’re not alone.” It’s a comforting and common refrain in a society that has increasingly embraced the importance of mental health. Yet, for all this growing awareness, the truth is that too many Americans are lonely. According to the American Psychological Association, more than half of U.S. adults feel isolated, left out, and stressed out by societal division.
In honor of Mental Health Awareness Month, Rula conducted its annual State of Mental Health Report to dive into trends on mental health and understand why many people have trouble accessing the care they need, despite growing awareness.
Based on responses from more than 2,000 U.S. adults, the 2026 report, “The Spaces Between Us: Navigating the Gaps, Traps and Barriers of Mental Health in America,” identifies:
Key trends shaping Americans’ mental health
Why and how people seek mental healthcare
Barriers that impact access to support
Check out the full 2026 State of Mental Health Report for more insights on mental health in the U.S.
Interested in exploring your mental health? Take the quiz to find your mental health support style:
Five major trends uncovered in Rula’s 2026 State of Mental Health Report
1. The attitude-behavior gap: Awareness isn't enough
Despite growing awareness of its importance, access to mental healthcare isn’t keeping pace with need. While nearly 60% of respondents report that mental health has become more important to them in the last five years, reported access to mental health services has slightly declined, from 50% in 2025 to 47.4% in 2026. This means that 52.6% of U.S. adults haven’t accessed services like talk therapy or psychiatry.
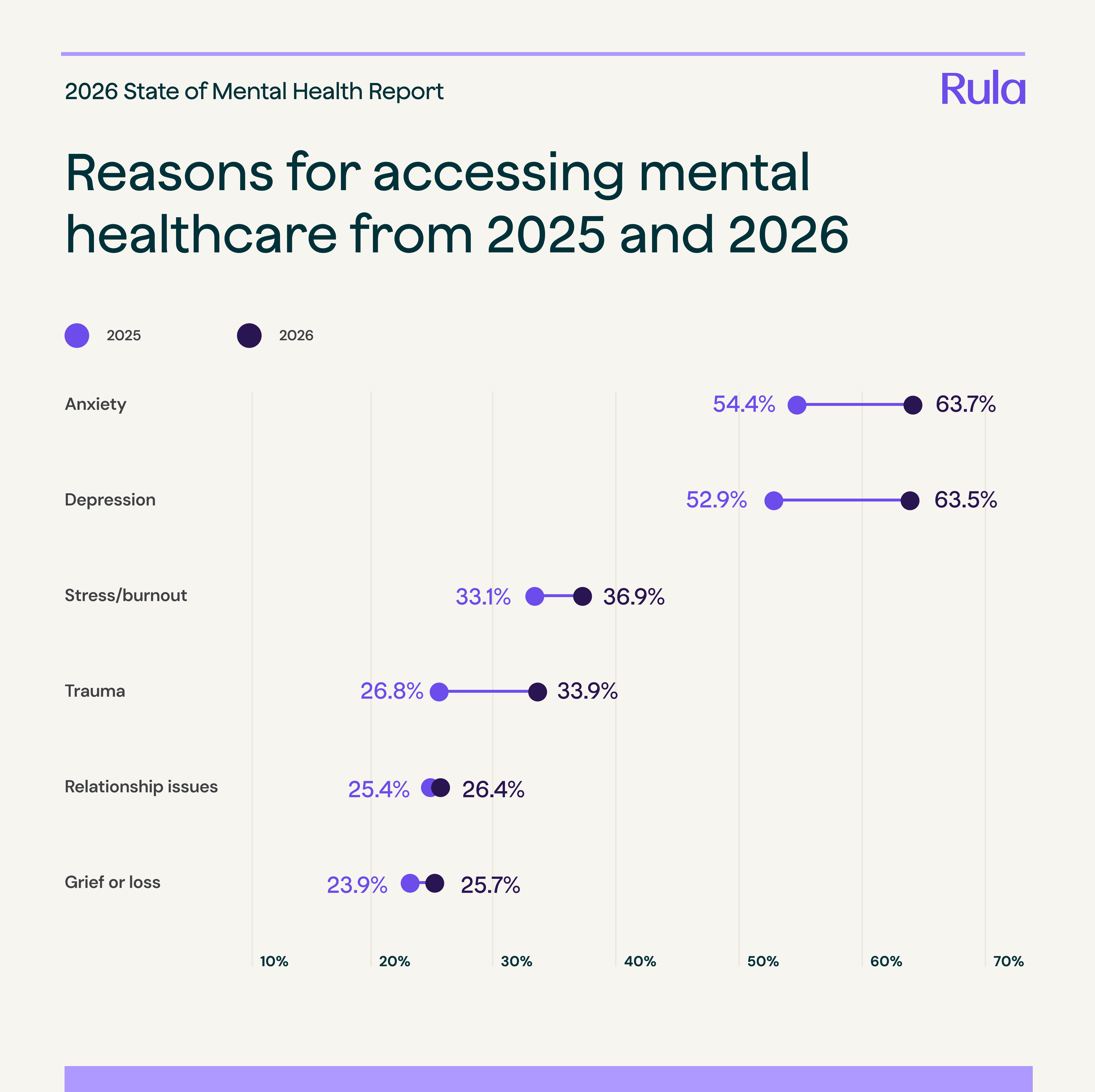
Yet, there’s a growing need for mental healthcare, as shown by the rising incidence of common mental health issues. The top reasons people seek support all increased from 2025 to 2026, with some rising over 10%. These include:
Anxiety (63.7%; +9.3% increase)
Depression (63.5%; +10.6% increase)
Stress or burnout (33.9%; + 3.8% increase)
Grief or loss (25.7%; +7.1% increase)
Anxiety and depression rose by 9.3% and 10.6%, respectively, between 2025 and 2026, and stress/burnout and trauma rose by 3.8% and 7.1%.
Although 81% of Americans now recognize the importance of mental health, awareness alone isn’t enough for everyone to get the help they might need. While many understand that therapy might help them, they often lack the confidence to take the first step.
The two most significant barriers to care are:
Cost, which was cited by more than 1 in 4 respondents
"Finding the right therapist," which was reported as a barrier by 19% of respondents
Education about mental health support options also presents a hurdle, as roughly 37% of respondents are unsure what kind of therapy would be most beneficial for them. In addition, many people don’t know how to track their moods and mental health symptoms, which could help them decide if therapy is right for them. When we asked people whether they track their mental health, the most common response was, "I don't keep track."
Many Americans are looking for social permission to access care. Having people in your circle who are openly speaking about and/or seeking mental health support is the single most powerful external motivator, cited by nearly half of all respondents (47%). Encouragement from family and friends to pursue mental healthcare was a close second, at 41% (a 5.3% increase from 2025).
2. The financial multiplier: A cycle of vulnerability
The increasing cost of living and an unstable job market are deeply affecting Americans' ability to access mental healthcare, as many struggle to cover basic expenses. The report reveals that 34% of Americans experience high financial stress, worrying about their finances daily or weekly.
This financial burden is directly impacting healthcare choices. For example, half of all respondents have reduced spending on therapy, gym memberships, or personal health due to rising costs. And a significant 54% feel exhausted from constantly trying to make their finances stretch.
These results show that those who need care most are often the least able to afford it. Both this year and last year, we found that cost was the leading obstacle to seeking support. The financial barrier to mental healthcare is getting more extreme, as it was cited by 41% of respondents in 2026 — a sharp increase from just 25% in 2025.
For people earning less than $50K annually, the high financial stress rate jumps to 42%. We also found that financial pressure is itself a reason to seek help, with 19.8% of Americans looking for mental health support specifically to address financial difficulties.
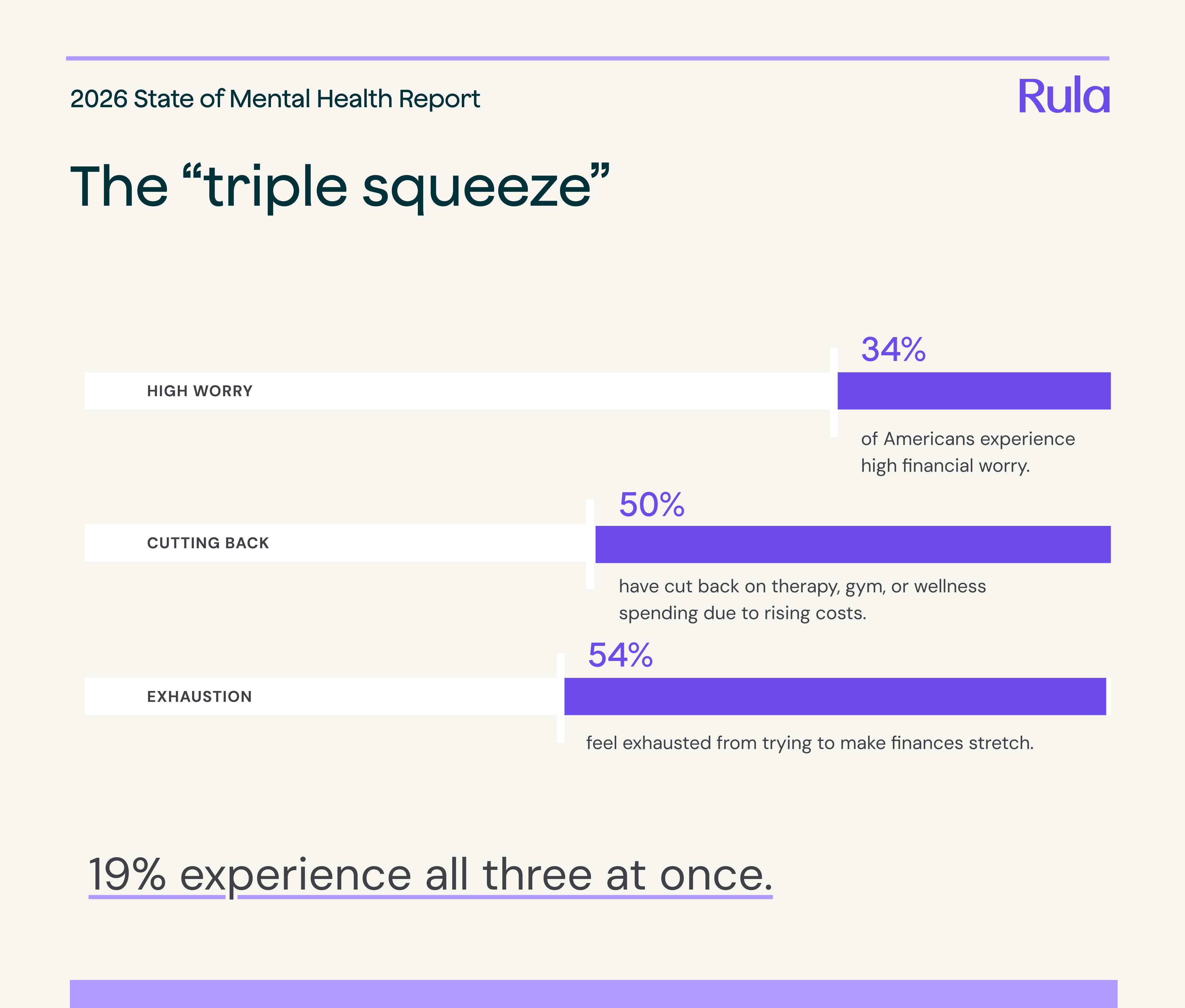
The report identifies a concerning "triple squeeze" affecting financially stressed Americans seeking mental health support:
34% experience high financial worry
50% have cut back on health-related services due to rising costs
54% feel exhausted from stretching their finances
19% experience all three of the above factors at once
When people struggle financially to meet their basic needs, the perceived cost of traditional therapy might be too great. But this untreated stress can compound, creating a vicious cycle of vulnerability that’s tough to escape without resources.
3. The gender gap: Matching complexity to care
The report highlights a significant gap in how men and women interact with mental healthcare.
As a group, women consistently engage more with mental health services. They are:
22% more likely than men to have ever accessed care
31% more likely than men to currently be in care
Women also seek support for common concerns at notably higher rates. They are:
13% more likely to seek support for anxiety
10% more likely for depression
21.6% more likely for trauma-related concerns
10.6% more likely for stress or burnout
While higher reported rates of anxiety and depression in women may partially explain this increased engagement, it may also point to a stigma that relies on masculinity norms to discourage men from seeking help. Despite this higher engagement, women report significantly lower improvement rates in therapy (71%) compared to men (81%).
This gap suggests that the current mental health system may not be designed for people with complex needs.
Women are 76% more likely than men to cite four or more reasons for seeking care, which may mean that their mental health challenges tend to be more complex. To make things even more complicated, women are 40% more likely to cite an inability to find the right therapist as a barrier. In fact, women often cycle through four or more providers before they find a suitable match.
However, the complexity of women’s mental health concerns might present an opportunity to create systems that provide better patient matching. For example, women using Rula’s online matching system to filter therapists according to their preferences typically meet just one or two providers before finding the right fit.
Improving mental health outcomes for everyone requires a system that provides better provider-patient matches, especially given the complex needs reported by women.
4. Beneath the mask: Mental health in the workplace
While organizations have made strides in diminishing mental health stigma and expanding wellness benefits, a significant gap remains between policy and truly healthy workplace.
Our report reveals that 43% of respondents have avoided telling their manager about a mental health challenge.
When employees mask these issues, they’re often bottling up emotions and creating inner turmoil that can impact their work. This could also cause them to miss out on vital at-work support, as managers are trained to advocate for their employees by adjusting workloads, clarifying benefits, or fostering team connections. Disclosing a mental health challenge could give employees the "social permission" they need to seek care.
Our research also highlights critical cultural and structural tensions, showing notable disparities:
Women are more likely than men to leave or consider leaving their jobs due to mental health concerns, despite being more inclined to seek care.
Gen Z is 6x more likely than Gen X to hide their mental health situations at work.
Though Gen Z is lauded for mental health awareness, this openness often doesn't extend to the workplace. As the youngest cohort, they may fear that showing vulnerability could be seen by management as a performance risk.
Among people who frequently hide their mental health at work:
81% miss work
28% miss 6+ days of work
79% consider quitting
Among people who never hide their mental health at work:
20% miss work
4% miss 6+ days of work
17% consider quitting
Workplace stigma is a clear operational risk. To bridge the gap, employers must proactively make mental health support visible, accessible, and normalized. This means actively marketing resources, reducing friction in accessing care, and ensuring support is available without mandatory disclosure.
5. The new technology frontier: AI in mental healthcare
The mental healthcare landscape is evolving, with many Americans seeking support from alternative sources. A significant finding from our survey is that more than 1 in 5 Americans have used AI chatbots for mental health support.
This trend isn't driven by a simple preference for technology, but rather by the desire for emotional safety and lower barriers to entry. The top reasons respondents gave for turning to AI were:
Feels more anonymous: 41%
Is less intimidating than therapy: 39%
Is more affordable: 35%
I prefer digital communication: 32%
I’m not comfortable face to face: 28%
Despite increasing concerns that AI might replace human clinicians, our data suggests a more complementary role. Seventy-one percent of AI therapy users have also been in traditional therapy, indicating that AI is expanding the reach of care to those already open to receiving it, rather than pulling people away from established services.
However, skepticism remains, and with good reason. Research from MIT highlights that using AI alone for mental health support may not be reliable and can potentially worsen feelings of loneliness. Americans are largely divided on AI's overall impact: 31% are hopeful, 34% are anxious, and 34% are neutral.
Paving the way for accessible mental healthcare with Rula
Rula is dedicated to making high-quality mental healthcare more accessible and affordable, serving as a comprehensive behavioral health solution.
We believe that this commitment begins with readily available, excellent care. By investing in data-integrated and measurement-informed care, we aim to improve outcomes and ensure people are matched with the appropriate provider.
Furthermore, we believe in the power of shared positive care experiences to ignite broader community conversation and encourage individual action, ultimately empowering more people to seek support. We are firm in the conviction that financial barriers or time constraints should never prevent people from accessing the care they need.
Find care with Rula
Choosing between mental health platforms is an important decision — one that shapes not just your access to care, but your entire experience of getting better. If you're ready to move forward with clarity and confidence, Rula makes it straightforward to connect with the right provider through your insurance.
You can verify your coverage and see your estimated costs upfront, browse providers who match your specific needs and preferences, and often book your first appointment as soon as tomorrow. When you're ready to take the next step, Rula is here to guide you to care that works.
Rula’s editorial process
Rula’s editorial team is on a mission to make science-backed mental health insights accessible and practical for every person seeking to better understand or improve mental wellness.
Members of Rula’s clinical leadership team and other expert providers contribute to all published content, offering guidance on themes and insights based on their firsthand experience in the field. Every piece of content is thoroughly reviewed by a clinician before publishing.





